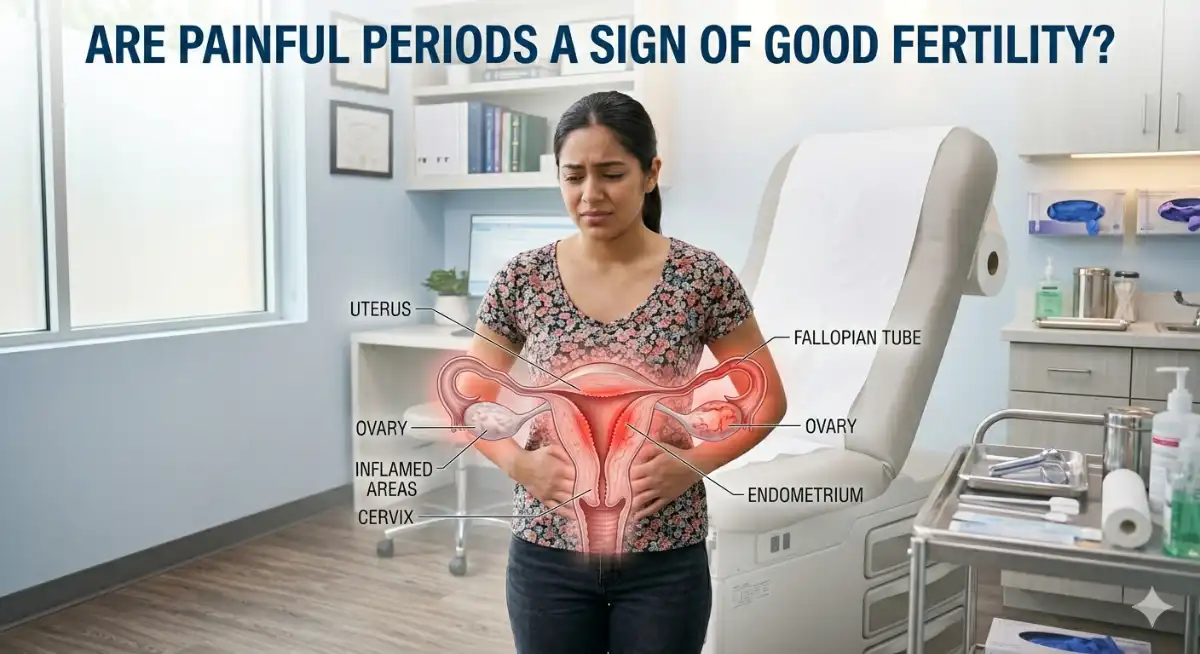
When discussing fertility and menstrual health, a common question arises: are painful periods a sign of good fertility? In 2026, with growing awareness around reproductive health, we now understand that menstrual pain (dysmenorrhea) is not a straightforward indicator of fertility. Instead, it reflects underlying hormonal, structural, or physiological factors that may or may not be related to reproductive potential.
We must clarify that fertility depends on ovulation quality, hormonal balance, uterine health, and overall reproductive function, not simply the presence or intensity of menstrual pain. While some women with strong cramps conceive easily, others with minimal discomfort may struggle with infertility—and vice versa.
What Causes Painful Periods?
To evaluate whether pain is linked to fertility, we must first understand its causes. Painful periods typically result from uterine contractions triggered by prostaglandins, hormone-like substances that regulate inflammation and muscle contraction.
Primary Dysmenorrhea
This is the most common type and occurs without any underlying disease. It is often associated with:
- Higher prostaglandin levels
- Strong uterine contractions
- Pain during ovulatory cycles
In such cases, the presence of ovulation may suggest that the reproductive system is functioning normally—but this does not automatically equate to high fertility.
Secondary Dysmenorrhea
This type results from medical conditions such as:
- Endometriosis
- Uterine fibroids
- Adenomyosis
- Pelvic inflammatory disease (PID)
These conditions can cause severe pain and negatively impact fertility, making painful periods a possible warning sign rather than a positive indicator.
Is Painful Menstruation a Sign of Ovulation?
Many believe that more pain means stronger ovulation, but this is only partially accurate. Painful periods can occur in cycles where ovulation happens, as prostaglandin levels rise after ovulation. However:
- Ovulation can occur without any pain
- Pain can occur even in anovulatory cycles
- Severe pain may indicate hormonal imbalance or pathology
Therefore, while some level of discomfort may coincide with ovulatory cycles, it is not a reliable fertility marker.
Hormones, Pain, and Reproductive Health
Fertility is deeply influenced by hormonal regulation. Painful periods are often linked to hormonal fluctuations, particularly:
- Estrogen dominance
- Progesterone deficiency
- Elevated prostaglandins
While these factors may cause intense cramps, they do not necessarily enhance fertility. In fact, hormonal imbalance can impair ovulation, reduce egg quality, and disrupt implantation.
A healthy reproductive system is characterized by:
- Regular menstrual cycles
- Balanced hormone levels
- Minimal to moderate discomfort
Excessive pain may signal that these systems are not functioning optimally.
Can Severe Period Pain Indicate Fertility Problems?
In many cases, severe menstrual pain is more closely associated with fertility challenges than fertility strength. Conditions like endometriosis, for example, are a leading cause of infertility and are often marked by:
- Intense pelvic pain
- Pain during intercourse
- Heavy or irregular bleeding
Similarly, fibroids and adenomyosis can distort the uterine environment, making implantation difficult.
Thus, rather than viewing pain as a positive sign, we must consider it as a potential indicator of underlying reproductive issues that may require medical evaluation.
Painful Periods vs. Healthy Cycles: What Truly Matters
When assessing fertility, we prioritize indicators that reflect reproductive health more accurately than pain levels. These include:
1. Regular Cycle Length
A consistent cycle (typically 21–35 days) suggests stable hormonal function.
2. Predictable Ovulation
Ovulation tracking through basal body temperature or ovulation kits provides better insight into fertility than pain.
3. Cervical Mucus Quality
Fertile cervical mucus (clear, stretchy) indicates optimal conditions for sperm survival.
4. Menstrual Flow Characteristics
A normal flow—not excessively heavy or extremely light—indicates uterine health.
Pain alone does not provide reliable data on any of these critical fertility markers.
Does Mild Period Pain Mean Low Fertility?
Another misconception is that less pain equals poor fertility. This is incorrect. Many women with painless or mildly uncomfortable periods have excellent fertility.
In fact, minimal pain often reflects:
- Balanced hormone levels
- Healthy uterine function
- Absence of inflammatory conditions
Therefore, lack of pain is not a negative sign—it may actually indicate a well-regulated reproductive system.
Lifestyle Factors That Influence Period Pain and Fertility
Modern research in 2026 emphasizes the role of lifestyle in both menstrual pain and fertility outcomes. Factors include:
Diet and Nutrition
- Diets high in processed foods and sugar can increase inflammation
- Nutrients like omega-3 fatty acids, magnesium, and vitamin B6 help reduce cramps
Physical Activity
- Regular exercise improves blood flow and reduces prostaglandin buildup
- Sedentary lifestyles may worsen menstrual discomfort
Stress Levels
- Chronic stress disrupts hormonal balance
- Elevated cortisol can interfere with ovulation
Sleep Quality
- Poor sleep impacts hormone regulation and reproductive health
Improving these areas can reduce pain and enhance fertility simultaneously, without relying on pain as an indicator.
When Should We Be Concerned About Painful Periods?
While mild discomfort is common, certain symptoms require attention:
- Severe pain that interferes with daily life
- Pain that worsens over time
- Irregular or excessively heavy bleeding
- Pain during intercourse
- Difficulty conceiving after 12 months of trying
These signs suggest that medical evaluation is necessary to rule out underlying conditions affecting fertility.
Modern Fertility Insights in 2026
Advancements in reproductive medicine have shifted the focus away from myths and toward measurable indicators. In 2026, fertility assessment includes:
- Hormone testing (AMH, FSH, LH)
- Ultrasound imaging of ovaries and uterus
- Ovulation tracking technologies
- Genetic and metabolic screening
These tools provide accurate insights into reproductive health, making subjective symptoms like pain less relevant as diagnostic indicators.
Final Verdict: Are Painful Periods a Sign of Good Fertility?
We conclude with clarity: painful periods are not a reliable sign of good fertility. While mild cramps may occur in healthy ovulatory cycles, moderate to severe pain often indicates inflammation, hormonal imbalance, or underlying medical conditions that could impair fertility.
The most accurate approach is to evaluate:
- Cycle regularity
- Ovulation consistency
- Hormonal balance
- Overall reproductive health
Rather than relying on menstrual pain as a signal, we must focus on comprehensive reproductive indicators supported by modern medical understanding.
Conclusion: Shift the Focus from Pain to Health
In today’s informed landscape, we move beyond outdated assumptions. Fertility is not measured by discomfort—it is defined by balance, function, and health. Painful periods should not be celebrated as a sign of reproductive strength; instead, they should be understood, evaluated, and managed appropriately.
By prioritizing accurate indicators and maintaining a healthy lifestyle, we can optimize fertility outcomes without relying on misleading myths.